Question 8#
Patients taking nonsteroidal anti-inflammatory drugs (NSAIDs) or aspirin need concomitant acid suppressing medication if which of the following is present?
A. Age over 50B. Heavy smoking history
C. Concurrent steroid intake
D. Heavy alcohol consumption
Correct Answer is C
Comment:
The overall risk of significant serious adverse gastrointestinal ( GI) events in patients taking nonsteroidal anti-inflammatory drugs (NSAIDs) is more than three times that of controls (Table below). This risk increases to five times in patients older than 60 years. Factors that clearly put patients at increased risk for NSAID-induced GI complications include age >60, prior GI event, high NSAID dose, concurrent steroid intake, and concurrent anticoagulant intake. Alcohol is commonly mentioned as a risk factor for peptic ulcer disease (PUD), but confirmatory data are lacking. High doses of H2 blockers have been shown to be less effective than proton pump inhibitors (PPis) in preventing GI complications in these high risk patients on antiplatelet therapy, but clearly they are better than no acid suppression.
Hospitalization rates for Gl events with and without NSAID use in selected large populations:
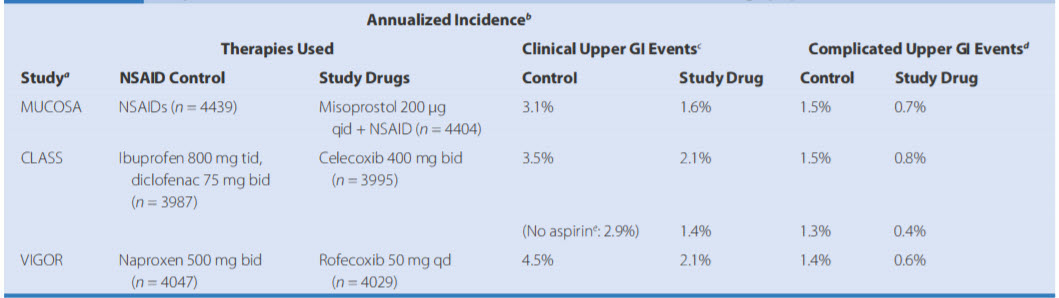
aMUCOSA and VIGOR trials included only rheumatoid arthritis patients; CLASS trial included osteoarthritis (73%) and rheumatoid arthritis (27%). blncidence for MUCOSA trial represents doubling of resu lts provided at 6 months (a lthough median follow-up was <6 months). Incidences for VIGOR and CLASS trials represent rates per 100 patient-years, although VIGOR median follow-up was 9 months and CLASS data include only the first 6 months of the study. cIncludes perforations, obstructions, bleedi ng, and uncomplicated ulcers discovered on clinically indicated work-up. dIncl udes perforation, obstruction, bleeding (documented due to ulcer or erosions in MUCOSA and CLASS; major bleeding in VIGOR). e21% of patients in CLASS study were taking low-dose aspirin. Note: All differences between controls and study drugs were significant except clinical upper Gl events in overall CLASS study (P = .09).