Question 2#
A 76-year-old woman, with past medical history of hypertension, coronary artery disease, atrial fibrillation, and Parkinson disease is admitted to the ICU with progressively worsening mental status. She suffered a ground level fall 2 days before her admission. Her home medications are amlodipine, lisinopril, levodopa, and apixaban. On physical examination, she is somnolent, only opens her eyes to painful stimuli, pupils are equal in size and briskly reactive to light, does not vocalize, and withdraws from noxious stimuli in all four extremities. The patient is emergently intubated for airway protection and admitted to the ICU. On arrival to the ICU, a head CT is obtained (see figure below).
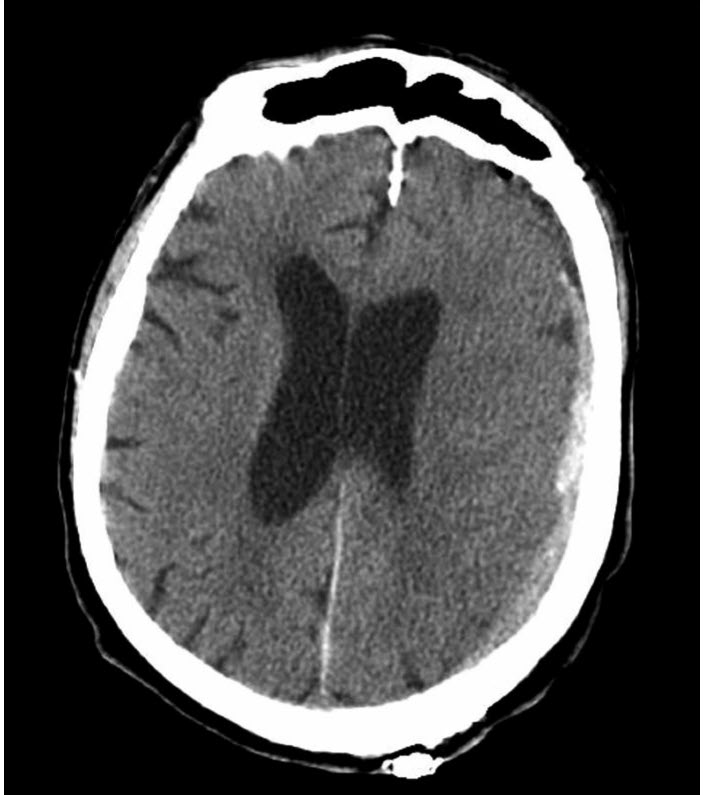
What will be the MOST appropriate next step in treatment?
A. Administer stat IV levetiracetamB. Administer stat IV mannitol
C. Administer stat IV NaCl 3%
D. Neurosurgical consultation for hematoma evacuation
Correct Answer is D
Comment:
Correct Answer: D
This patient has the classic presentation of SDH, with the gradual neurological deterioration after a fall. Imaging reveals a L. hemispheric SDH, primarily acute but probably with some chronic components (lesshyperintense areas). Head CT also demonstrates left-sided cerebral edema with left to right midline shift. Although seizures are very common in SDH patients, the description does not suggest a current seizure. It is common to administer prophylactic, not therapeutic doses of an antiepileptic medication (Answer A is incorrect). Although imaging does show significant cerebral edema with a midline shift, osmotherapy is generally avoided as it may cause further shrinkage of the brain tissue, which will expand the subdural space and exacerbate the bleed (Answers B and C are incorrect).
The correct answer is D: in an acute, symptomatic SDH, the solution is surgical evacuation. The patient requires a clot evacuation in the operating room as soon as possible.
References:
- Fomchenko EI, Gilmore EJ, Matouk CC, et al. Management of subdural hematomas: part I. medical management of subdural hematomas. Curr Treat Options Neurol. 2018;20:28.
- Fomchenko EI, Gilmore EJ, Matouk CC, et al. Management of subdural hematomas: part II. surgical management of subdural hematomas. Curr Treat Options Neurol. 2018;20:34.