Question 2#
A 51-year-old male with a recent history of acute pericarditis 6 weeks ago now resents with new onset chest pain. He stopped high-dose ibuprofen 4 weeks ago and has been feeling well since then. The chest pain started 12 hours ago, is very sharp, substernal, and pleuritic in nature. The symptoms are similar to his prior episode of pericarditis. He denies palpitations, lightheadedness, orthopnea, shortness of breath, and lower extremity edema.
On physical examination:
- he is afebrile
- pulse of 104 beats per minute
- blood pressure 134/68 mm Hg
- room air oxygen saturation of 99%
He has an audible friction rub. Kussmaul sign and jugular venous distension are absent. Laboratory evaluation reveals two negative serial troponin values, normal white blood cell count and creatinine, and mildly elevated C-reactive protein. ECG has nonspecific changes without ST-segment elevation. Echocardiogram shows normal biventricular function, no wall motion abnormalities, and a trace pericardial effusion that was previously visualized as well.
What is the most appropriate next therapy?
A. Heparin bolus and dripB. Corticosteroids
C. Broad spectrum antibiotics
D. High dose ibuprofen and colchicine
E. Anakinra
Correct Answer is D
Comment:
Correct Answer: D
Approximately 15% to 30% of patients with idiopathic acute pericarditis will have a recurrence. Recurrent pericarditis is diagnosed with new symptoms of pericarditis after resolution of prior symptoms, signs of persistent pericardial inflammation (ECG changes, elevation of CRP, friction rib, new or worse pericardial effusion) after a symptom-free period of 4 weeks or more from the prior episode of pericarditis. This patient has a history of pericarditis and presents with acute onset chest pain similar to his prior episode of pericarditis. A nonspecific ECG and negative troponins with 12 hours of chest pain decreases the likelihood of acute coronary syndrome, and thus heparin not indicated. The similarity of symptoms to prior pericarditis, friction rub, and elevated CRP occurring 4 weeks after stopping ibuprofen all point toward recurrent pericarditis as the cause of his chest pain. First line therapy for recurrent pericarditis consists of reinitiating highdose NSAIDs along with colchicine. NSAID therapy should be continued until complete resolution of symptoms and objective signs of pericarditis (CRP normalization, etc.), and then tapered. Colchicine should be continued for the duration of NSAID therapy. It improves response to NSAID and reduces the risk of recurrence by half. Proton pump inhibitor should be prescribed for gastric protection from NSAIDs. Exercise restriction is also reinstated until resolution of symptoms and normalization of CRP.
In the presence of contraindications to NSAIDs and colchicine, or recurrence of pericarditis during NSAID/colchicine therapy, low-dose corticosteroids can be considered as second line therapy, after exclusion of infectious causes. Prednisone at doses of 0.2 to 0.5 mg/kg/d (or equivalent other steroid dosing) may be considered for at least 2 to 4 weeks, and until symptoms and signs resolve. Once remission has been achieved, the steroids should be gradually tapered over 2 to 4 weeks. Next line therapies include immunosuppressive medications such as azathioprine, anakinra (a recombinant anti-interleukin-1 receptor antagonists), and intravenous immunoglobulin infusions.
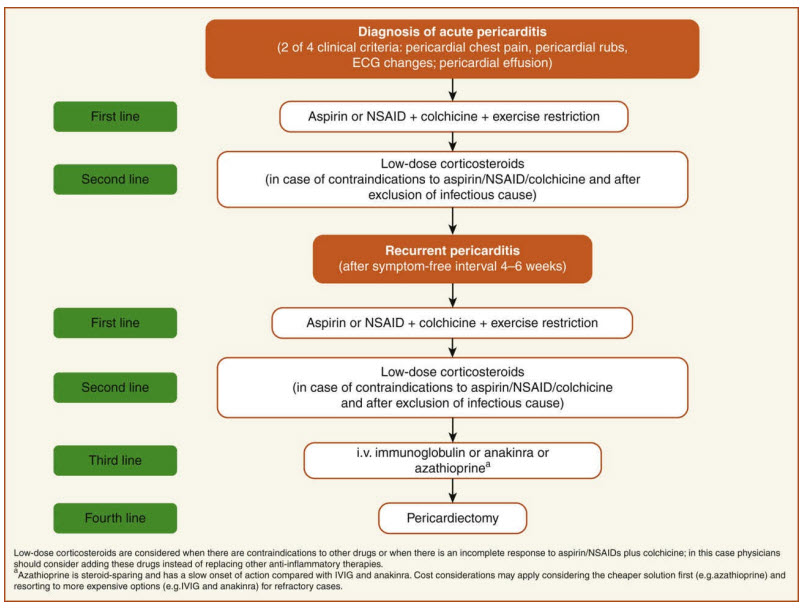
(Figure from Adler Y, Charron P, Imazio M, et al. 2015 ESC guidelines for the diagnosis and management of pericardial diseases: the task force for the diagnosis and management of pericardial diseases of the European Society of Cardiology (ESC). Eur Heart J. 2015;36:2921.)
References:
- Lilly LS. Treatment of acute and recurrent idiopathic pericarditis. Circulation. 2013;127:1723-1726.
- Zipes DP, Libby P, Bonow RO, Mann DL, Tomaselli GF, Braunwald E. Braunwald’s Heart Disease: A Textbook of Cardiovascular Medicine. 11th ed. Philadelphia, PA: Elsevier/Saunders; 2018.