Question 4#
A 75-year-old male with a past medical history significant for severe aortic stenosis is admitted to the surgical intensive care unit for acute posthemorrhagic anemia secondary to a lower GI bleed. Lower endoscopy reveals angiodysplasias of the ascending colon that were subsequently cauterized. The next day the patient has additional bloody bowel movements. Laboratory test results show:
- platelet count of 120,000
- hemoglobin of 7.2
- PTT of 42
What is the most definitive treatment for this patient?
A. FFPB. Desmopressin
C. Repeat Endoscopy with cauterization
D. Aortic Valve Replacement
Correct Answer is D
Comment:
Correct Answer: D
The patient’s presentation is most likely Heyde syndrome. First noticed in 1958, the triad includes moderate to severe aortic stenosis or calcified aortic valves, bleeding from arteriovenous malformations in the colon, and acquired von Willebrand disease (vWD). The different vWD Types are shown in table below:
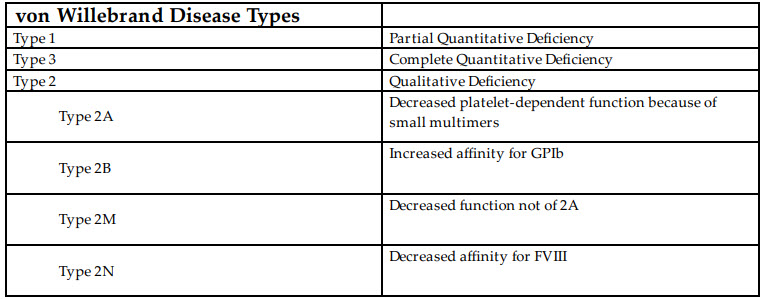
Acquired vWD or vWD 2A occurs in numerous disease processes. The various etiologies include hematologic cancers, solid tumors (Wilm’s), and extremely turbulent areas of blood flow with a sufficient proportion of total blood flow to cause significant disruption of total circulating von Willebrand Factor (vWF) (eg aortic stenosis).
The pathogenesis of vWD IIA in aortic stenosis is uncoiling of the vWF multimer. When uncoiled by shear stress the site at which ADAMTS13 (vWF cleaving protease) cleaves the vWF multimer is exposed, resulting in shorter vWF strands with decreased function in primary hemostasis and enhanced clearance. The clinical impact is persistent bleeding from mucosal tissues, in this case, from colonic angiodysplasia.
Laboratory test result values will be mostly normal with either a normal or slightly prolonged PTT due to the physical association of vWF and factor VIII. However, the PTT cannot be used to rule-out vWF deficiency. Temporizing measures include administration of FFP or desmopressin. Although data are limited in the case of recurrent bleeding from Heyde syndrome, aortic valve replacement could offer definitive management.
References:
- Pate GE, Mulligan A. An epidemiological study of Heyde’s syndrome: an association between aortic stenosis and gastrointestinal bleeding. J Heart Valve Dis. 2004;13(5):713-716. Available at http://www.ncbi.nlm.nih.gov/pubmed/15473467.
- Godino C, Lauretta L, Pavon AG, et al. Heyde’s syndrome incidence and outcome in patients undergoing transcatheter aortic valve implantation. J Am Coll Cardiol. 2013;61(6):687-689. Available at https://www.sciencedirect.com/science/article/pii/S0735109712057130? via%3Dihub.
- Loscalzo J. From clinical observation to mechanism – heyde’s syndrome. N Engl J Med. 2012;367(20):1954-1956. Available at http://www.nejm.org/doi/abs/10.1056/NEJMcibr1205363.