Question 2#
A 22-year-old man presents with a 6-month history of a red, nonpruritic rash over the trunk, scalp, elbows, and knees. These eruptions are more likely to occur during stressful periods and have occurred at sites of skin injury. The patient has tried topical hydrocortisone without benefit. On examination, sharply demarcated plaques are seen with a thick scale. Pitting of the fingernails is present. There is no evidence of synovitis.
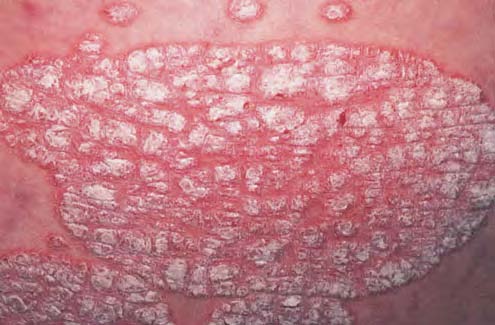
What is the best first step in the therapy of this patient’s skin disease?
A. Photochemotherapy (PUVA)B. Oral methotrexate
C. Topical calcipotriene
D. Oral cyclosporine
E. Topical betamethasone
Correct Answer is E
Comment:
The rash described is classic for psoriasis, a common chronic inflammatory skin disorder. Its characteristic features include sharply bordered papules or plaques with silver scale, usually located on the knees, elbows, and scalp. Stress, certain medications such as lithium, and skin injury commonly exacerbate the disease. The distribution of the described rash would make contact dermatitis unlikely. In the differential of psoriasis are lichen planus (polygonal pruritic purple papules with lacy mucous membrane lesions), pityriasis rosea (herald patch on trunk, spreading in a Christmas tree pattern), and dermatophytes (usually less well demarcated; affecting skin, hair, and nails). Topical corticosteroids of moderate or high potency are the first agents to try in psoriasis without joint involvement.
Topical vitamin D analogues such as calcipotriene or calcitriol may be combined with topical steroids in refractory cases, but they are less effective and much more expensive than topical steroids. Psoralens with UVA phototherapy (PUVA) are reserved for moderate to severe widespread cases because of an increased risk of squamous cell carcinoma of the skin. Methotrexate, cyclosporine, and immune response modifiers such as etanercept are useful in difficult cases, but carry a higher risk of side effects.